
ACR BI-RADS® ATLAS — BREAST MRI
American College of Radiology 125
MAGNETIC RESONANCE
IMAGING
III. REPORTING SYSTEM

2013
126 American College of Radiology
MAGNETIC RESONANCE
IMAGING

ACR BI-RADS® ATLAS — BREAST MRI
American College of Radiology 127
MAGNETIC RESONANCE
IMAGING
A. REPORT ORGANIZATION
The reporting system should be concise and organized. Any pertinent clinical history that may af-
fect scan interpretation, as well as any MRI acquisition techniques (including postprocessing informa-
tion) that may aect the scan interpretation, should be described. The breast MRI report should rst
describe the amount of broglandular tissue and the background parenchymal enhancement (BPE).
Abnormal enhancement (unique and separate from the BPE) is described based on morphology,
distribution, and kinetics. Results from any physiologic or parametric imaging should be described.
An assessment is rendered that includes the degree of concern and any recommendation(s). Benign
ndings need not be reported, especially if the interpreting physician is concerned that the referring
clinician or patient might infer anything other than absolute condence in benignity.
Table 2. Report Organization
Report Structure
1. Indication for examination
2. MRI technique
3. Succinct description of overall breast composition
4. Clear description of any important ndings
5. Comparison to previous examination(s)
6. Assessment
7. Management
1. INDICATION FOR EXAMINATION
Provide a brief description of the indication for examination. For example, this may be high-risk
screening, follow-up of a probably benign lesion, follow-up of cancer treated with neoadjuvant
chemotherapy, or evaluation of the newly diagnosed cancer patient.
As background parenchymal enhancement can be aected by cyclical hormonal changes, it may
be helpful to include menstrual history. If the patient is pre-menopausal, the week of the menstrual
cycle may be important information to aid in interpretation. Current therapy (neoadjuvant, adju-
vant, hormonal, or radiation therapy) for breast cancer treatment in the pre-or postsurgical setting
may be important information and may inform exam interpretation.
The indication for examination should contain a concise description of the patient’s clinical his-
tory, including:
a. Reason for performing the exam (e.g., screening, staging, problem solving)
b. Clinical abnormalities, including size, location, and duration
i. Palpable nding
ii. Nipple discharge
iii. Other pertinent clinical ndings or history

2013
128 American College of Radiology
MAGNETIC RESONANCE
IMAGING
c. Previous biopsies
i. Biopsy type
ii. Biopsy location
iii. Benign or malignant pathology (cytology or histology)
d. Hormonal status if applicable
i. Pre- or post-menopausal
ii. Menstrual cycle phase (second week or other) or last menstrual period
iii. Peripartum
iv. Exogenous hormone therapy, tamoxifen, aromatase inhibitors, or other hormones or
medications/herbs/vitamins that might inuence MRI
2. MRI TECHNIQUE
Give a detailed description of the technical factors of how the MRI examination was obtained. At a
minimum, a bright-uid sequence of both breasts should be obtained. Pre- and post-gadolinium
T1-weighted images should be obtained, preferably with fat suppression, simultaneously of both
breasts. Subtraction imaging may be desired as well as other as processing techniques and para-
metric analysis. Elements of this description routinely include:
a. Right, left, or both breasts
b. Location of markers and their signicance (scar, nipple, palpable lesion, etc.)
c. Weighting
i. T1 weighted
ii. T2 weighted
iii. Fat saturation
iv. Scan orientation and plane
v. Other pertinent pulse sequence features
d. Contrast dose
i. Name of contrast agent
ii. Dosage (mmol/kg) and volume (in cc)
iii. Injection type: bolus or infusion
iv. Timing (relationship of bolus injection to scan start time and scan length)
v. If multiple scans: number of postcontrast scans and acquisition techniques of each (how
fast, how many slices, and slice thickness)
e. Postprocessing techniques as applicable
i. MPR/MIP
ii. Time/signal intensity curves
iii. Subtraction
iv. Other techniques
ACR BI-RADS® ATLAS — BREAST MRI
American College of Radiology 129
MAGNETIC RESONANCE
IMAGING
3. SUCCINCT DESCRIPTION OF OVERALL BREAST COMPOSITION
This should include an overall description of the breast composition, including:
a. The amount of FGT that is present
Table 3. Breast Tissue — Fibroglandular Tissue (FGT)
Amount of Fibroglandular Tissue
a. Almost entirely fat
b. Scattered broglandular tissue
c. Heterogeneous broglandular tissue
d. Extreme broglandular tissue
The four categories of breast composition (Table 3) are dened by the visually estimated
content of FGT within the breasts. If the breasts are not of apparently equal amounts of FGT
the breast with the most FGT should be used to categorize breast composition. Although
there may be considerable variation in visually estimating breast composition, categorizing
based on percentages (and specically into quartiles) is not recommended. We recognize
that quantication of breast FGT volume on MRI may be feasible in the future, but we await
publication of robust data before endorsing percentage recommendations. We urge the
use of BI-RADS® terminology instead of numbers to classify breast FGT in order to eliminate
any possible confusion with the BI-RADS® assessment categories, which are numbered.
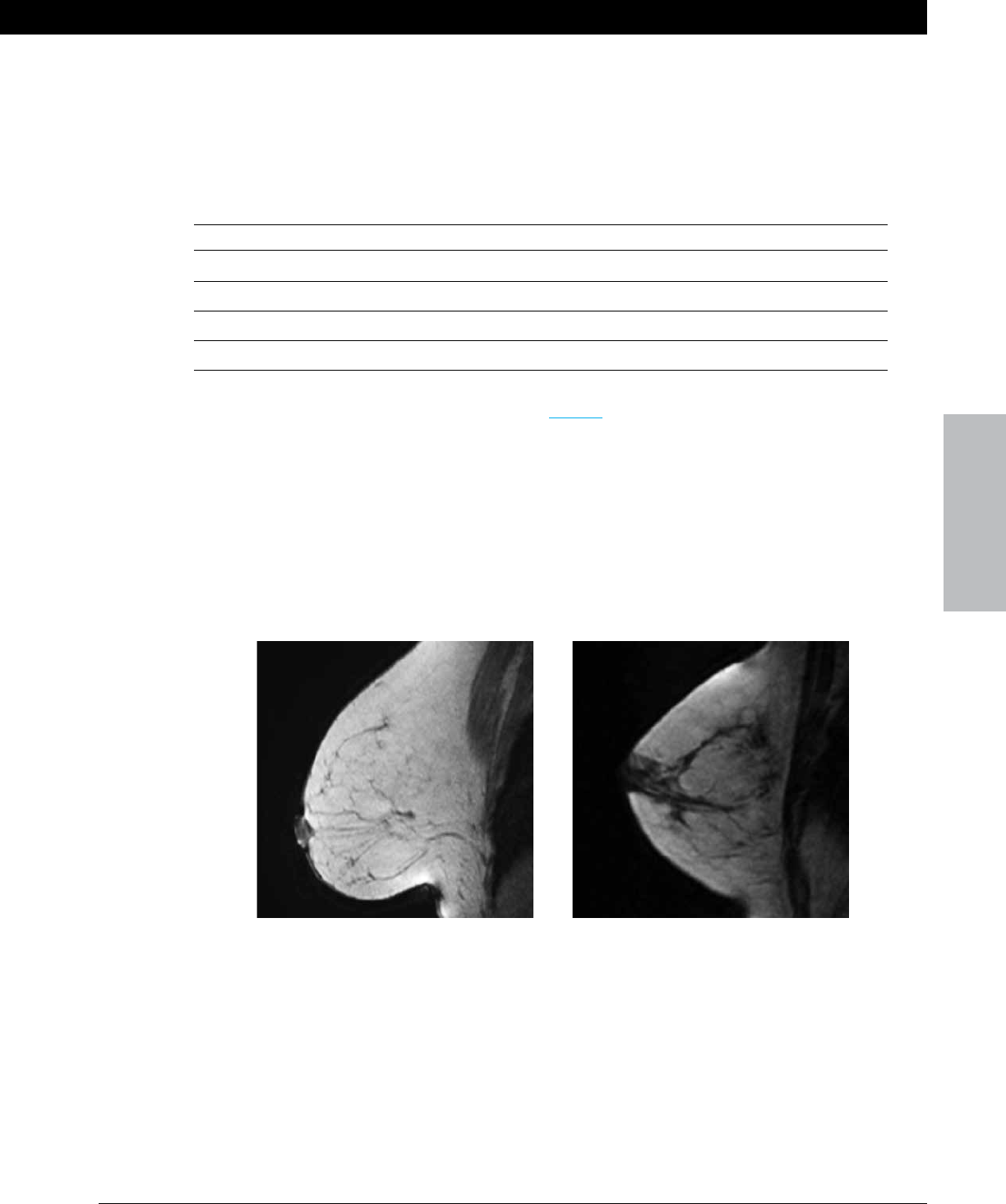
Figure 262 – Almost entirely fat. Figure 263 – Scattered broglandular tissue.

2013
130 American College of Radiology
MAGNETIC RESONANCE
IMAGING
Figure 264 – Heterogeneous broglandular
tissue.
Figure 265 – Extreme broglandular tissue.
b. The amount of background parenchymal enhancement in the image
Table 4. Breast Tissue — Background Parenchymal Enhancement (BPE)
Background Parenchymal Enhancement
a. Minimal
b. Mild
c. Moderate
d. Marked
The four categories of BPE (Table 4) are dened by the visually estimated enhancement of
the FGT of the breast(s). If the breasts are not of an apparently equal amounts of BPE, the
breast with the most BPE should be used to categorize BPE. In the event that treatment has
altered BPE in one or both breasts, this can be reported. Although there may be considerable
variation in visually estimating BPE, categorizing based on percentages (and specically into
quartiles) is not recommended. Quantication of BPE volume and intensity on MRI may be
feasible in the future, but we await publication of robust data on that topic before endorsing
percentage recommendations. We recognize that there are variations in BPE distribution and
morphology. However, we defer on recommending descriptions of distribution or morphol-
ogy until additional data are available. Currently, BPE refers to the volume of enhancement
and the intensity of enhancement. For consistency, BPE should be included for all patients,
using the categories in Table 4.

ACR BI-RADS® ATLAS — BREAST MRI
American College of Radiology 131
MAGNETIC RESONANCE
IMAGING
Figure 268 – Moderate. Figure 269 – Marked.
Figure 266 – Minimal. Figure 267 – Mild.
On bilateral scans, describe whether the pattern is asymmetric or symmetric, if appropri-
ate. Asymmetric denotes more enhancement in one breast than in the other. Symmetric
enhancement is mirror image.
c. Whether implants are present
If an implant is present, it should be so stated in the report. Information should include its
composition (saline, silicone, or other) and the number of lumens (single or multiple).

2013
132 American College of Radiology
MAGNETIC RESONANCE
IMAGING
4. CLEAR DESCRIPTION OF ANY IMPORTANT FINDINGS
Abnormal enhancement is unique and separate from BPE. Its description should indicate the
breast in which the abnormal enhancement occurs, the lesion type, and modiers.
The clinical location of the abnormality as extrapolated from the MRI location (based on clock-face
position and quadrant location) should be reported. It should be recognized that there may be
variation in location of a clinically detected lesion (patient is upright or supine), a mammographi-
cally detected lesion (patient is upright and compressed), a sonographically detected lesion (pa-
tient is supine or supine oblique), and an MRI-detected lesion (patient is prone) based on positional
dierences. A more consistent measurement is the distance from the nipple. It is encouraged that
distance from the nipple for a lesion be reported in order to facilitate correlation between modali-
ties, although it should be understood that one should expect some dierence in distance from
the nipple among the breast imaging modalities.
For bilateral axial examinations, the breasts should be pointing up, following the cross-sectional
imaging convention.
The descriptors should include:
a. Size
b. Location
i. Right or left
ii. Breast quadrant and clock-face position (or central, retroareolar, and axillary tail descriptors)
iii. Distance from nipple, skin, or chest wall in centimeters (if applicable)
Descriptors for abnormal enhancement:
c. Findings associated with abnormal enhancement include:
i. Artifacts that aect interpretation
ii. Focus: a tiny dot of enhancement that does not clearly represent a space-occupying le-
sion or mass and does not clearly show a mass on precontrast imaging.
iii. Masses: space-occupying lesions, usually spherical or ball-like, may displace or retract
surrounding breast tissue
Descriptors — modiers describing a mass:
(a) Shape: describes the overall morphology of the enhancement
Oval (includes lobulated)
Round
Irregular
(b) Margin: describes the borders
Circumscribed
Not circumscribed
o Irregular
o Spiculated

ACR BI-RADS® ATLAS — BREAST MRI
American College of Radiology 133
MAGNETIC RESONANCE
IMAGING
(c) Internal enhancement characteristics
Homogeneous
Heterogeneous
Rim enhancement
Dark internal septations
iv. Non-mass enhancement (NME): modiers describing enhancement patterns with a specic
MRI pattern
(a) Distribution
Focal
Linear
Segmental
Regional
Multiple regions
Diuse
(b) Internal enhancement patterns (for all other types)
Homogeneous
Heterogeneous
Clumped
Clustered ring
v. Intramammary lymph node (rarely important)
vi. Skin lesion (rarely important)
vii. Non-enhancing ndings
(a) Ductal precontrast high signal on T1W
(b) Cyst
(c) Postoperative collections (hematoma/seroma)
(d) Post-therapy skin thickening and trabecular thickening
(e) Non-enhancing mass
(f) Architectural distortion
(g) Signal void from foreign bodies, clips, etc.
viii. Associated features
(a) Nipple retraction
(b) Nipple invasion
(c) Skin retraction

2013
134 American College of Radiology
MAGNETIC RESONANCE
IMAGING
(d) Skin thickening
(e) Skin invasion
Direct invasion
Inammatory cancer
(f) Axillary adenopathy
(g) Pectoralis muscle invasion
(h) Chest wall invasion
(i) Architectural distortion
ix. Fat-containing lesions
(a) Lymph nodes
Normal
Abnormal
(b) Fat necrosis
(c) Hamartoma
(d) Postoperative seroma/hematoma with fat
x. Stability: describe how the enhancement changed (if new, stable, or changed in size
from previous examination)
xi. Kinetic curve assessment (if applicable)
(a) The fastest enhancing portion of the lesion or the most suspicious washout curve
pattern in the lesion should be assessed
Sample fast enhancing areas
Sample for and report on the worst looking kinetic curve shape
(b) Signal intensity/time curve
Initial enhancement phase – describes the enhancement pattern within the rst
2 minutes or when the curve starts to change
o Slow
o Medium
o Fast
Delayed phase – describes the enhancement pattern after 2 minutes or after the
curve starts to change
o Persistent
o Plateau
o Washout

ACR BI-RADS® ATLAS — BREAST MRI
American College of Radiology 135
MAGNETIC RESONANCE
IMAGING
xii. Implants
(a) Implant material and lumen type
Saline
Silicone
o Intact
o Ruptured
Other implant material (such as soy oil, polypropylene, polyurethane, and sponges;
includes direct injections)
Lumen type
(b) Implant location
Retroglandular
Retropectoral
(c) Abnormal implant contour
Focal bulge
(d) Intracapsular silicone ndings
Radial folds
Subcapsular line
Keyhole sign (teardrop, noose)
Linguine sign
(e) Extracapsular silicone
Breast
Lymph nodes
(f) Water droplets
(g) Peri-implant uid
Also, we recognize that other techniques may be used in the evaluation of breast lesions. Newer
and evolving techniques are constantly being introduced. Findings from other techniques, such
as diusion-weighted imaging or MR spectroscopy, should be reported if clinically important.

2013
136 American College of Radiology
MAGNETIC RESONANCE
IMAGING
5. COMPARISON TO PREVIOUS EXAMINATION(S)
Include a statement indicating that the current examination has been compared to previous
examination(s) with specic date(s). If this is not included, it should be assumed that no com-
parison has been made; however, it is preferable to indicate explicitly that no comparison was
made. Comparison to a previous examination may assume importance if the nding of concern
requires an evaluation of change or stability. Comparison is less important when the nding has
characteristically benign features. Comparison may be irrelevant if the nding is inherently sus-
picious for malignancy. Information in this area should include:
a. Previous MRI — date of examination
b. Other imaging studies (mammogram, US, nuclear medicine examination, other) and date of
examination
6. ASSESSMENT
This is a description of an overall summary of MRI ndings, including assessment.
Incorporating an assessment category in the overall summary of the breast MRI report is sound
medical practice. All nal impressions should be complete with each lesion fully categorized.
An incomplete assessment (category 0) is used when full diagnostic imaging has not been per-
formed and should be given only when additional imaging or clinical evaluation is recommended
to establish the benignity of a nding (e.g., a possible intramammary lymph node or fat necrosis at
MRI may require additional mammography and/or US examination).
Interpretation is facilitated by recognizing that almost all MRI examinations may be classied into a
few assessment categories, listed in the section on Assessment Categories. (See page 137)
7. MANAGEMENT
This is a description of patient management recommendations, as appropriate.
If an incomplete assessment (category 0) is rendered, a specic suggestion for the next course
of action should be given (physical examination, diagnostic mammography, targeted diagnostic
US, etc.). Note that an incomplete assessment (category 0) should not be rendered when rec-
ommending targeted US in order to determine the feasibility of performing biopsy using sono-
graphic guidance; such a scenario requires the use of a category 4 or 5 assessment (suspicious or
highly suggestive of malignancy).
If a suspicious abnormality is detected, the report should indicate that a biopsy should be per-
formed in the absence of clinical contraindication. This means that the radiologist has sucient
concern that a biopsy is warranted; the term “clinical contraindication” indicates that there may be
reasons why the patient and her physician might wish to defer the biopsy.

ACR BI-RADS® ATLAS — BREAST MRI
American College of Radiology 137
MAGNETIC RESONANCE
IMAGING
1. ASSESSMENT IS INCOMPLETE
Category 0: Incomplete — Need Additional Imaging Evaluation
Use this for a nding that needs additional imaging evaluation. This may be used for a technically
unsatisfactory scan or when more information is needed to interpret the scan. A recommenda-
tion for additional imaging evaluation might involve a repeat MRI with satisfactory technique or
obtaining information with other imaging modalities (mammographic views, US, etc.). The radi-
ologist should use judgment in how vigorously to pursue previous studies.
Every eort should be made not to use category 0. The reason for this is that almost always there
is enough information on the initial breast MRI examination to provide a management recom-
mendation. In general, the decision to biopsy or not may be made on the basis of the existing
MRI study. A situation in which a nal assessment of 0 may be helpful is when a nding on MRI is
suspicious, but demonstration that the nding is characteristically benign on an additional study
would avert biopsy. For example, if a small mass is suspicious on MRI but there is a possibility that
it may represent a benign nding, such as an intramammary lymph node, then a category 0 as-
sessment may be made, with the recommendation for targeted US (that might demonstrate char-
acteristically benign features) to possibly avert biopsy. Another example would be a suspicious
nding at MRI that may represent fat necrosis, with the recommendation for diagnostic mam-
mography (that might demonstrate characteristically benign features) to possibly avert biopsy. If
a category 0 assessment is rendered at MRI, detailed recommendations should describe the sub-
sequent diagnostic imaging workup and the level of suspicion (pertinent in case the additional
imaging does not establish benignity).
When additional studies are completed, a nal assessment is rendered. If the additional studies
are described in the same report, separate paragraphs indicating the pertinent ndings from
each imaging study will contribute to the nal integrated assessment that takes all the ndings
into consideration.
Table 5. Concordance Between BI-RADS® Assessment Categories and Management Recommendations.
Assessment Management Likelihood of Cancer
Category 0: Incomplete — Need
Additional Imaging Evaluation
Recommend additional imaging:
mammogram or targeted US
N/A
Category 1: Negative
Routine breast MRI screening if
cumulative lifetime risk ≥ 20%
Essentially 0% likehood of ma-
lignancy
Category 2: Benign
Routine breast MRI screening if
cumulative lifetime risk ≥ 20%
Essentially 0% likehood of ma-
lignancy
Category 3: Probably Benign
Short-interval (6-month) follow-up
≥ 0% but ≤ 2% likehood of malig-
nancy
Category 4: Suspicious
Tissue diagnosis
> 2% but < 95% likehood of
malignancy
Category 5: Highly Suggestive of
Malignancy
Tissue diagnosis
≥ 95% likehood of malignancy
Category 6: Known Biopsy-Proven
Malignancy
Surgical excision when clinically
appropriate
N/A
B. ASSESSMENT CATEGORIES
The assessment categories are based on BI-RADS® categories developed for mammography.

2013
138 American College of Radiology
MAGNETIC RESONANCE
IMAGING
2. ASSESSMENT IS COMPLETE FINAL ASSESSMENT CATEGORIES
Category 1: Negative
There is nothing to comment on. This is a normal examination.
No abnormal enhancement was found; routine follow-up is advised. There is nothing to com-
ment on. The breasts are symmetric, and no enhancing masses, architectural distortion, or sus-
picious areas of enhancement are present.
Category 1 includes a normal description of breast composition (amount of FGT) and the de-
gree of BPE. It should be emphasized that BPE is a normal nding, and short-term follow-up is
not necessary to assess BPE for stability.
Category 2: Benign
Like category 1, this is a normal assessment, but here the interpreter chooses to describe a
benign nding in the breast MRI report. The interpreter may describe a benign nding such as:
intramammary lymph node, implants, metallic foreign bodies (such as core biopsy and surgical
clips), enhancing and non-enhancing broadenomas, cysts, old non-enhancing scars or recent
scars; postoperative collections, fat-containing lesions (such as oil cysts, lipomas, galactoceles,
and hamartomas). On the other hand, the interpreter may choose not to describe such nd-
ings, in which case the examination should be assessed as negative (category 1). Both category
1 and 2 assessments indicate that there is no evidence of malignancy. The dierence is that
category 2 should be used when describing one or more specic benign MRI ndings in the
report, whereas category 1 should be used when no such ndings are described (even if such
ndings are present).
The committee supports a directive for annual follow-up MRI and mammography after either
a category 1 or 2 screening MRI assessment, in line with established guidelines for high-risk
screening.
Category 3: Probably Benign
A nding assessed using this category should have a ≤ 2% likelihood of malignancy, but greater
than the essentially 0% likelihood of malignancy of a characteristically benign nding. A prob-
ably benign nding is not expected to change over the suggested period of imaging surveil-
lance, but the interpreting physician prefers to establish stability of the nding before recom-
mending management limited to routine breast screening.
Although data are becoming available that shed light on the ecacy of short-interval follow-up
for selected MRI ndings, at the present time, such management recommendations are based
on limited data. The use of a probably benign (category 3) assessment is reserved for specic
ndings that are separate from the BPE and are very likely benign. The use of a category 3 as-
sessment has been intuitive in the past; however, there are several studies.
1,2,3
that specically
address rates of malignancy and, to a very limited extent, types of lesions. Although these stud-
ies examined dierent populations of patients, several of them were able to demonstrate a
≤ 2% malignancy rate, demonstrating the feasibility of using category 3 assessments at MRI.
However, none of the studies provided PPVs for specic types of lesions, so the use of category
3 assessment at MRI remains intuitive for radiologists who lack extensive (audited) personal
experience with any given specic type of lesion. Currently, this is an evolving area that needs
the support of robust data before an unqualied endorsement is made to use category 3 as-
sessments at MRI.

ACR BI-RADS® ATLAS — BREAST MRI
American College of Radiology 139
MAGNETIC RESONANCE
IMAGING
As at mammography, if a probably benign nding is smaller or less prominent (i.e., less contrast
enhancement) on follow-up examination, the nding should be assessed as benign (category 2),
eliminating the need for continued surveillance imaging. When a nding that otherwise meets
probably benign imaging criteria is either new or has increased in size, extent, or conspicuity, then
a recommendation for biopsy would be prudent and a recommendation for follow-up should not
be rendered.
BPE, a benign nding on nearly all MRI examinations, should not be the reason for a probably be-
nign assessment. However, if ndings cannot be ascribed to normal variation of BPE and there is a
question about whether observed enhancement could be transient and related to the hormonal
status of the patient, then a probably benign (category 3) assessment with a recommendation to
return for very-short-interval follow-up (2–3 months) may be appropriate.
Because a benign hormonal enhancement can vary from cycle to cycle, a category 3 assess-
ment may be used for the menstruating patient who was scanned in a suboptimal phase of her
cycle; a follow-up MRI examination should be scheduled for the optimal (week 2) phase of her
cycle. Additionally, a category 3 assessment may be used for the post-menopausal patient who
is on hormone replacement therapy (HRT) and in whom probable hormonal enhancement is
observed. Stopping HRT for several weeks and repeating the scan may be warranted in this sce-
nario. It should be emphasized that unexplained areas of enhancement that are demonstrated
to be due to HRT are uncommon. As with mammography, if the nding is smaller or less promi-
nent (i.e., less contrast enhancement) at follow-up examination, the nding is benign.
Recommendations will likely undergo future modications as more data accrue regarding the
validity of using category 3 assessments at MRI, the follow-up interval required, and the type of
ndings that should be followed.
Follow-up of Foci
Foci are dened as small dots of enhancement that are unique and stand out from the BPE.
They are too small to be accurately assessed with respect to margin or internal enhance-
ment. Indeed, if margin or internal enhancement can be assessed, the nding should be
considered a small mass and not a focus. New foci or foci that have increased in size should
be viewed with suspicion and carefully evaluated.
Correlation with bright-uid imaging (T2W imaging or STIR imaging) can be helpful in the
evaluation of a focus. If a correlate is uniformly very high in signal intensity or if cyst-like fea-
tures are identied, the focus may be assessed as benign. (Most of these foci represent lymph
nodes or small myxomatous broadenomas.) However, if the focus does not have a very high
signal correlate on bright-uid imaging, then the focus may or may not be benign. These foci
may be followed or biopsied. In certain cases (if the nding is new or increased in size) the
focus always should be biopsied. Note that malignant foci may be brighter than the surround-
ing FGT, although they do not usually appear cyst-like.
Follow-up of Masses
Masses that enhance and are identied on an initial MRI examination should undergo assess-
ment based on morphology and kinetics. It has been documented that occasionally malig-
nancy may demonstrate benign-appearing MRI features, such as an oval or round shape with
a circumscribed margin and homogeneous internal enhancement. Therefore, in a scenario in
which the stability of the nding is unknown, periodic surveillance imaging may be appropri-
ate, depending on various factors that aect the prior probability of malignancy (age, cancer
risk, etc.) as well as the patient’s willingness to accept surveillance imaging as an alternative to

2013
140 American College of Radiology
MAGNETIC RESONANCE
IMAGING
biopsy, given less than robust data that support a watchful waiting approach. If surveillance
imaging is undertaken, an increase in size of the mass should prompt immediate biopsy.
Follow-up of NME
NME that is unique and separate from the overall background enhancement should undergo
assessment based on morphology and kinetics. Bright-uid imaging sequences can be helpful
in these instances to demonstrate any associated cysts, which may support a diagnosis of fo-
cal brocystic change and a benign (category 2) assessment. However, limited data on linear,
clumped, and segmental enhancement indicate that these ndings should not be followed,
as the malignancy rate appears to be greater than 2%.
4
At this time, the literature is not suf-
ciently robust to endorse the use of a category 3 assessment for NME.
Timing of Follow-up
Final assessment category 3 is best used for a unique focal nding and managed with an initial
short-interval follow-up (6 months) examination followed by additional examinations until long-
term (2- or 3-year) stability is demonstrated. For category 3 assessments, the initial short-term
follow-up interval is usually 6 months, involving the breast(s) containing the probably benign
nding(s). Assuming stability at this 6-month examination, a category 3 assessment again will
be rendered with a management recommendation for a second short-interval follow-up exami-
nation in 6 months, but now involving both breasts if the opposite breast will be due for routine
annual screening. Again assuming stability at this second short-interval follow up, the examina-
tion is once more assessed as category 3, but now the recommended follow-up interval usually
is lengthened to 1 year due to the already-observed 12-month stability. The recommended 2- or
3-year follow-up in these cases is: 6 months, 6 months, 1 year, and, optionally, 1 more year to es-
tablish stability. After 2 to 3 years of stability, the nding should be assessed as benign (category
2). It should be emphasized that this approach is borrowed from mammography. While the vast
majority of probably benign ndings are managed with follow-up, there may be occasions in
which biopsies are done instead (patient preference or overriding clinical concern). As with any
interpretive examination, a less experienced reader may conclude that a nding such as benign
BPE, for example, should be classied as category 3. A more experienced reader may recognize
this as normal or benign at 6 or 12 months and classify it as category 1 or 2. With a properly
worded report, the assessment category may then be changed to one that the current reader
feels is appropriate, even though long-term stability has not been demonstrated.
It is imperative that surveillance imaging does not alter the stage at diagnosis or prognosis
of the few patients with malignancies who are given category 3 assessments. Because this
has not yet been demonstrated for MRI, as it has been for mammography, careful audit-
ing of the use of category 3 assessments is necessary, and publication of outcomes data
is strongly recommended. Although the data are not robust, it appears the ≤ 2% malig-
nancy rate already demonstrated at mammographic follow-up also may be achieved at
MRI. Several recent publications have demonstrated that focal lesions assigned to category
3 had a ≤ 2% malignancy rate, albeit without use of specic BI-RADS® MRI descriptors for
the lesions included in the studies.
5,6,7
Publication of outcomes data for specic category
3 lesions, using BI-RADS® MRI, is strongly recommended. It should be noted that a ≤ 2%
malignancy rate may be dicult to achieve due to the high-risk population that usually is
studied by MRI (higher than average prior probability of cancer).
A desirable goal for the frequency of making category 3 assessments at MRI is less than 10%.
Over time, this rate should decrease to the point that a mature program should demonstrate

ACR BI-RADS® ATLAS — BREAST MRI
American College of Radiology 141
MAGNETIC RESONANCE
IMAGING
a rate much closer to the approximately 1%–2% rate currently achieved at mammography,
especially as the availability of previous examination(s) increases. A decrease in the frequency
of category 3 assessments and false-positive outcomes has been demonstrated in the breast
MRI literature as experience is gained.
Category 4: Suspicious
This category is reserved for ndings that do not have the classic appearance of malignancy
but are suciently suspicious to justify a recommendation for biopsy. The ceiling for a cat-
egory 3 assessment is a 2% likelihood of malignancy and the oor for a category 5 assess-
ment is 95%, so category 4 assessments cover the wide range of likelihood of malignancy in
between. Thus, almost all recommendations for breast interventional procedures will come
from assessments made using this assessment category. In breast MRI, assessment category
4 is not currently divided into subcategories 4A, 4B, and 4C.
Category 4 is used for the majority of ndings prompting breast intervention, which can be
performed by percutaneous biopsy, by US or stereotactic guidance, or by MRI guidance for
lesions not visible at either US or mammography. As cysts rarely pose a problem in inter-
pretation at MRI, diagnostic aspiration is not commonly performed. In many patients with
a suspicious abnormality at MRI, targeted US will identify a corresponding abnormality so
that US-guided biopsy can be performed. US-guided biopsies are faster, more comfortable
for the patient, and more cost eective than MRI-guided biopsies. There are no established
guidelines on who should undergo targeted US. However, in general, patients with masses
larger than 5 mm should be examined by targeted US if the MR appearance is suspicious.
Areas of NME may be evident on US as well, thus bringing the radiologist’s judgment into
play. Factors that may limit visibility at US include fatty breasts, extremely complex breasts
with multiple cysts, very large breasts, and very deep lesions. If there is any question about
whether a presumed sonographic correlate actually is the same as the suspicious MRI lesion,
MR-guided biopsy is advised.
Category 5: Highly Suggestive of Malignancy
These assessments carry a very high probability (≥ 95%) of malignancy. This category ini-
tially was established to include lesions for which 1-stage surgical treatment was consid-
ered without preliminary biopsy, in an era when preoperative wire localization was the
primary breast interventional procedure. Nowadays, given the widespread acceptance of
imaging-guided percutaneous biopsy, 1-stage surgery rarely if ever is performed. Rather,
current oncologic management almost always involves tissue diagnosis of malignancy via
percutaneous tissue sampling. This facilitates treatment options, such as when sentinel
node biopsy is included in surgical management or when neoadjuvant chemotherapy is
administered prior to surgery. Therefore, the current rationale for using category 5 assess-
ment is to identify lesions for which any nonmalignant percutaneous tissue diagnosis is
considered discordant, resulting in a recommendation for repeat (usually surgical) biopsy.
No single MRI descriptor is suciently predictive of malignancy to produce the ≥ 95% prob-
ability required for a category 5 assessment. Just as in mammography and US, an appropriate
combination of suspicious ndings is needed to justify a category 5 assessment at MRI. It is rec-
ommended that category 5 assessments be audited separately to verify a ≥ 95% PPV, thereby
validating that the assessment is not being overused.

2013
142 American College of Radiology
MAGNETIC RESONANCE
IMAGING
Category 6: Known Biopsy-Proven Malignancy
This category is reserved for examinations performed after biopsy proof of malignancy (im-
aging performed after percutaneous biopsy) but prior to surgical excision, in which there are
no abnormalities other than the known cancer that might need additional evaluation. That
is, a cancer diagnosis has already been established, a lesion is depicted at MRI, and this lesion
corresponds to the previously biopsied cancer.
A category 6 is not appropriate following successful lumpectomy or mastectomy (margin
of resection free of tumor). The rationale for establishing category 6 is exclusion of these
cases from auditing, because additional malignancy is frequently found such that auditing
these cases would inappropriately skew overall outcomes. In the event that the breast with
known cancer has a separate suspicious MRI nding that requires biopsy for diagnosis, the
appropriate category 4 or 5 assessment should be rendered, and this would be the overall
assessment because it leads to more prompt intervention.

ACR BI-RADS® ATLAS — BREAST MRI
American College of Radiology 143
MAGNETIC RESONANCE
IMAGING
C. WORDING THE REPORT
The current examination should be compared to prior examinations when appropriate. The indica-
tion for examination, such as screening or diagnostic, should be stated. The report should be orga-
nized with a brief description of the composition of the breast and any pertinent ndings, followed
by the assessment and management recommendations. All discussions between the interpreting
physician and the referring clinician or patient should be documented in the original report or in an
addendum to the report.
The report should be succinct, using terminology from the approved lexicon without embellish-
ment. Do not use denitions of the lexicon terms in the report narrative; use only the descriptors
themselves. Following the impression section and the (concordant) management recommenda-
tions section of the report, the terminology for the assessment category should be stated, as well as
its category number. Other aspects of the report data should comply with the ACR Practice Guide-
line for Communication: Diagnostic Radiology.
REFERENCES
1. Weinstein SP, Hanna LG, Gatsonis C, Schnall MD, Rosen MA, Lehman CD. Frequency of malignancy seen in
probably benign lesion at contrast-enhanced breast MR imaging: ndings from ACRIN 6667. Radiology 2010;
255:731–7.
2. Eby PR, DeMartini WB, Peacock S, Rosen EL, Lauro B, Lehman CD. Cancer yield of probably benign breast MR
examinations. J Magn Reson Imaging 2007; 26:950–5.
3. Kriege M, Brekelmans CTM, Boetes C, et al. Ecacy of MRI and mammography for breast-cancer screening in
women with a familial or genetic predispodition. N Engl J Med 2004; 351:427–37.
4. Liberman L, Morris EA, Dershaw DD, Abramson AF, Tan LK. Ductal enhancement on MR imaging of the breast.
AJR 2003; 519–25.
5. Mahoney MC, Gatsonis C, Hanna L, DeMartini WB, Lehman CD. Positive predictive value of BI-RADS MR imag-
ing. Radiology 2012; 264:51–8.
6. Eby PR, DeMartini WB, Gutierrez RL, Lehman CD. Probably benign lesions detected on breast MR imaging.
Magn Reson Imaging Clin N Am 2010; 18:309–21.
7. Warner E, Plewes DB, Hill KA, Causer PA, et al. Surveillance of BRCA 1 and BRCA 2 mutation carriers with magnetic
resonance imaging, ultrasound, mammography, and clinical breast examination. JAMA 2004; 292:1317–25.
